In our Functional Rehab course, taught by Dr. Young, we’ve been practicing analyzing each other’s postures and gaits and applying specific functional movement tests to narrow down our hypotheses of syndromes and generate proper rehabilitation programs. At first, it’s challenging to look at one’s body and find the irregularities, but if you scan the body and analyze in sections, it becomes more apparent.

Left: Chris standing naturally, facing forward to assess his posture.
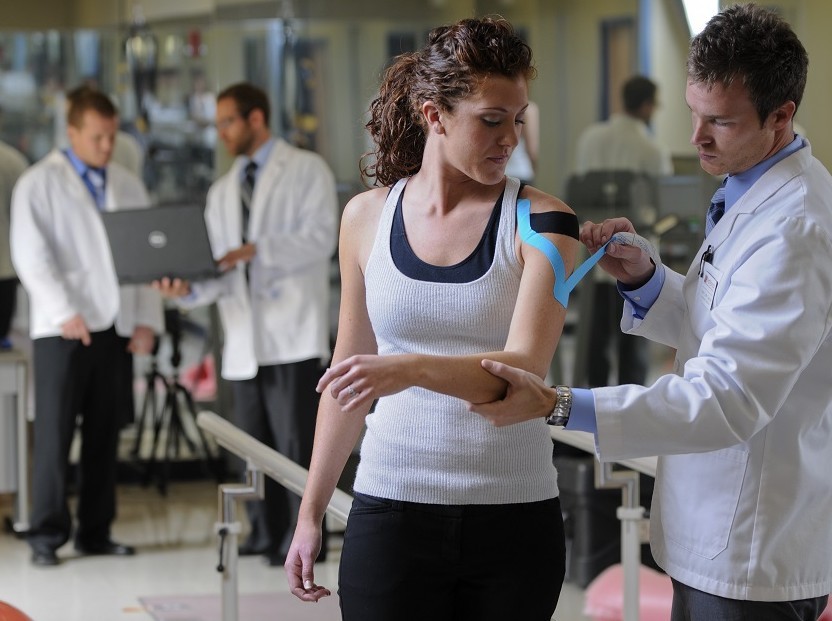
Right: Jared instructing Chris to perform a specific functional movement test.
In the image with Chris standing facing forward, one can see that his left shoulder sits higher than the other. He has a slight lateral head tilt to the left and his chin is elevated upwards. In a different view, one can see that he stands with his feet externally rotated (toes faced out) and he has pes planus on both feet. From a side view, he demonstrates anterior head translation and an anterior pelvic tilt. These postural findings suggest he may have Upper Cross syndrome, as well as Lower Cross Syndrome.
To further evaluate him, Chris naturally walked to-and-from a spot. During his gait, we could see that he overpronates, has calcaneal eversions, and a flat-foot contact on both feet. To better understand whether the dysfunction was a foot or hip problem, we asked Chris to perform several functional movement tests, such as a pelvic tilt test, single limb stance test, 6’’ step down test, and Jandas hip extension test.
Tests demonstrated that he has late gluteus maximus activation, weak deep abdominal muscles, bends his knees over toes while stepping down. This suggests that he has hip instability rather than foot instability. With this information, we can then perform manual muscles tests to determine whether the instability stems from a strength or coordination issue. In this case, Chris has a coordination issue. After palpating for segmental restrictions and muscular hypertonicity and completing range of motion movements, we can generate our rehabilitation plan by choosing specific soft tissue stretching techniques and exercises that would help improve Chris’s muscle coordination and improve his posture and gait.
Learning how to properly assess posture, gait, and functional movement tests will help us better understand how to evaluate future patients and determine proper rehab protocols to help them reach optimal wellness and health. By learning how to assess each other, this encourages us to each come up with our own conclusions while also enabling us to discuss our progress with classmates. It’s also a fantastic way for us to improve our own kinematic chain distortions and syndromes!
Learn more about studying to become a chiropractic physician here.